Floaters and Flashes
What are Floaters and Flashes in the Eye?
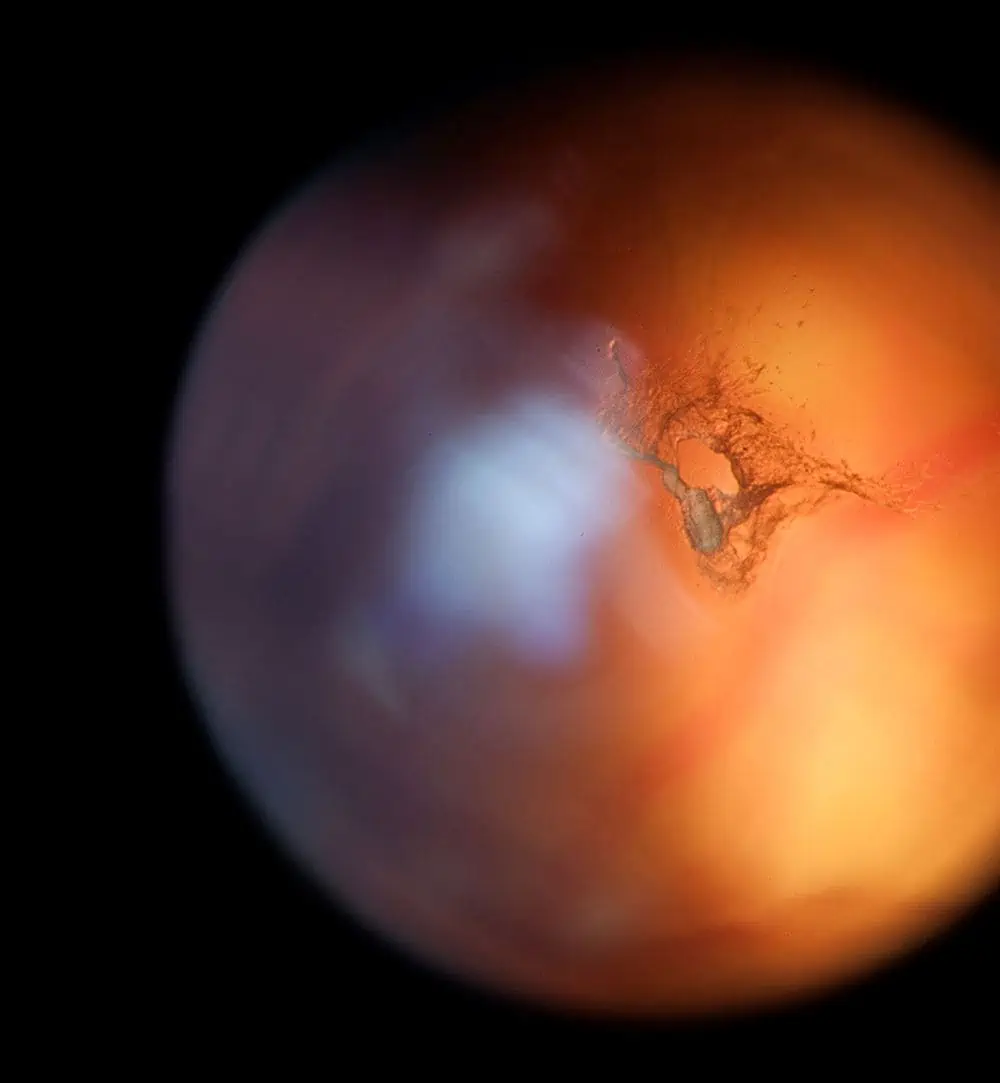
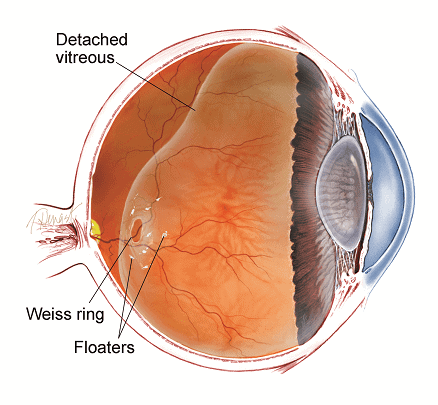
Small specks or clouds moving in the field of vision are called floaters. These are made up of tiny clumps of gel or cells inside the vitreous, the clear jelly-like fluid that fills the inside of the eye. When people reach middle age, the gel may start to thicken or shrink forming clumps or strands inside the eye. Floaters if present over a long time or increasing in number very slowly are usually harmless.
New floaters that come on suddenly or there is a substantial increase in them can be important. This may occur when the gel pulls away from the back of the eye and in some cases it causes the retina to tear. A torn retina is a serious problem.
When the vitreous gel inside the eye rubs or pulls on the retina, flashes of light may be seen. The flashes can occur on and off for weeks or months. Sudden flashes, however, may require immediate attention because it could mean that the retina has been torn.
Treatment of Floaters
Because there is a risk of a torn retina, it is recommended to see your eye specialist if a new floater or flashes appear suddenly. While some floaters may remain in your vision, many of them will fade over time and become less bothersome. In some patients, however, floaters can cause persistent, distracting and disabling symptoms and reading or driving become problems. Laser treatment can break-up large floaters to reduce the impact they have on vision or a surgical procedure called a vitrectomy may rarely be recommended.
Treatment for light flashes that are related to a torn retina may include laser photocoagulation or cryotherapy. These are usually done under local anaesthetic in the surgery. As with any surgery, there are risks that will be discussed with you by your surgeon.
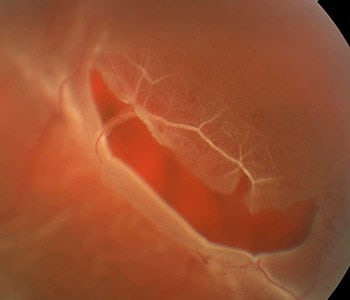
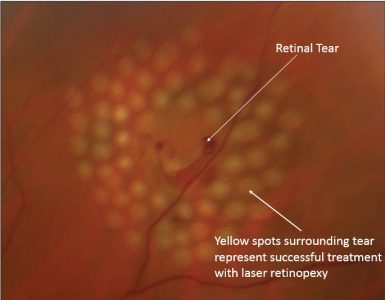
Retinal Tear
The retina is the light-sensing layer lining the inner surface at the back of the eye. When a retinal detachment occurs the retina is pulled away from the inner surface of the eye and fails to function properly. There is no pain associated with a retinal detachment. This can result in the patient seeing peripheral shadows, a curtainlike effect over the vision, flashes of light or dark spots, or total loss of vision in the affected eye. Early diagnosis and treatment are important to ensure the best outcome. Your surgeon will discuss with you and determine the best treatment option.
Possible causes of retinal detachment:
- Retinal tear or hole
- Trauma
- Advancing age
- Family history of retinal tear or detachment
- High level of myopia
- Eye surgery – such as cataract surgery
- Eye disease or inflammation
- Diabetes
Diagnosis of Retinal Detachment - examination involves
- Patient medical history
- Auto refraction
- Lensometer – measure glasses
- Visual Acuity – check vision using a Snellen eye chart
- Tonopen – check Intraocular pressure.
- Dilate the pupil
- Examination of the retina – this will require dilating eye drops
Treatment of retinal tear – treatment is aimed to close the retinal hole or tear and to prevent further damage and retinal detachment
Drainage of the subretinal fluid – in some instances the fluid trapped between the retina and choroid layers may be reabsorbed naturally without any treatment required. In some circumstances, however, the fluid may need to be drained by the surgeon.
Argon Laser (photocoagulation) – Laser to back of the eye (retina). Dilating eye drops are used Takes about 45 minutes. Light sensitivity and mild discomfort may be experienced and you should have someone drive you home after the procedure.
Cryotherapy – Cryotherapy uses an extremely cold probe applied to the outside of the eye in the area of the retinal tear. This ‘freezes’ the retina and choroid in place. This seal assists the eye to reattach the retina.
Treatment of retinal detachment
Pneumatic retinopexy – A small air or gas bubble is injected into the eye. The patient is required to position their head so that the bubble sits against the retinal detachment and presses the retina back onto the choroid layer. As the retina heals and re-attaches the gas bubble is reabsorbed over the next several weeks.
Scleral Buckle – A small band or ‘buckle’ of silicone is attached to the outside of the eye at the point of the detachment. As the buckle is fixed it causes an indentation in the eye pushing the retina back in contact with the eye. A scleral buckle is usually permanent.
Vitrectomy – This procedure is used to cut and remove the vitreous jelly that is pulling on the retina. It can also be used to remove any blood that may be clouding the vitreous or foreign matter from the eye if trauma has occurred. A vitrectomy involves making a series of small incisions into the eye to allow the probe to enter the back of the eye. In some cases, the vitreous removed may be replaced with silicone oil or other synthetic solution, or a gas bubble is used.
As with any surgery, there are risks that will be discussed with you by your surgeon.

